Think Your Baby Might Be Allergic to Cow’s Milk? Here’s What Parents Need to Know
It’s one of the most stressful moments for a new parent: your baby is fussy, spitting up, having diarrhea, maybe even showing blood in their stool. Then, your pediatrician mentions the possibility of a cow’s milk allergy and suddenly, you’re facing big changes like switching to expensive specialized formulas or cutting all dairy from your own diet if you’re breastfeeding.
Before you overhaul your pantry or say goodbye to cheese, here’s the truth: most babies diagnosed with cow’s milk allergy don’t actually have it.
The Two Types of Cow’s Milk Allergy
There are two main kinds of cow’s milk allergy:
IgE-mediated allergy
This is the “classic” food allergy caused by a specific immune response.
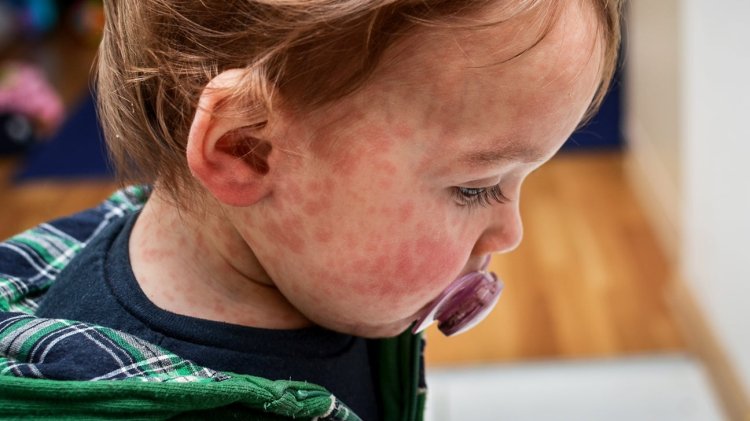
Symptoms can include rashes, facial swelling, hives, flushing, or difficulty breathing.
Blood tests and skin tests can help confirm this diagnosis.
Non-IgE-mediated allergy
This one is much trickier to diagnose.
Symptoms can include vomiting, diarrhea, blood in the stool, and fussiness during or after feeding.
The challenge? Many healthy babies have these symptoms for other reasons colic, reflux, or even a small tear in the anus.
The only reliable way to confirm a non-IgE cow’s milk allergy is to:

Remove all dairy from the diet.
See if symptoms improve.
Reintroduce dairy and check if symptoms return.
But here’s the catch: once a baby improves, many parents (understandably) never reintroduce dairy which means we can’t be sure it was the actual cause.
How Common Is Cow’s Milk Allergy, Really?
A special report in JAMA Pediatrics revealed a surprising fact:
While 14% of babies are reported to have cow’s milk allergy…
Only about 1% actually do.
Even more eye-opening: in 81% of published guidelines on cow’s milk allergy, the authors had ties to formula manufacturers. That doesn’t mean the advice is wrong but it does raise concerns about how recommendations are shaped.
The Reality for Breastfeeding Moms

If you’re breastfeeding, you’ve probably heard you must cut all dairy if your baby has a suspected allergy. But the latest research shows most breastfeeding mothers don’t need to eliminate dairy even if the allergy is IgE-mediated. Many are unnecessarily restricting their diets, risking their own nutrition, and in some cases, stopping breastfeeding entirely.
What Parents Should Do Before Making Big Changes
If your baby is fussy, vomiting, or having unusual stools, don’t panic. These issues are very common in newborns and infants and often resolve on their own.
Before changing formula or cutting dairy from your diet:
Ask your doctor exactly why they believe it’s a cow’s milk allergy.
Discuss testing options especially if symptoms suggest an IgE-mediated allergy.
If it’s suspected to be non-IgE mediated, talk about whether a carefully supervised elimination and reintroduction makes sense.
Never make major diet changes for you or your baby without guidance from your pediatrician.
The Bottom Line for Parents
Cow’s milk allergy is real but rare. While some babies truly need dietary changes, many improve with time, without switching formulas or eliminating dairy. The best thing you can do is ask questions, understand the reasoning, and get a clear diagnosis before making big (and costly) adjustments.
Parenting is already full of challenges let’s not add unnecessary restrictions to the list.
What's Your Reaction?